"Now faith is the substance of things hoped for, the evidence of things not seen."
Bob Nelson, MD
Forum for Healthcare Freedom
February 9, 2021
In late December 2020 and January 2021, our hopes were fulfilled when the first doses of COVID-19 vaccine were administered to front-line healthcare workers and other at-risk persons. Finally, a chance to compile real-world data on the protective effects of detectable antibody in vaccine recipients and those who recovered from the natural disease. Finally, a predicate to chart a path back to a life with handshakes and hugs.
Other than self-congratulatory rhetoric about rapid distribution of vaccine and the number of dosages administered, there has been mainly silence from our overseers about how our post-vaccine world should look. What we have heard, instead, are continued calls for social distancing and masks for an indeterminate period. To be fair, the vaccination process has only recently begun and the prudent path would be a gradual relaxing of restrictions. Yet, the absence of a conversation detailing a way out of this predicament seems to be a bizarre stance to take; especially considering the personal and societal price we have paid for long-term economic shutdowns and the multiple restrictions we have endured while waiting on a vaccine to save us.
For the entire Coronavirus pandemic, the “substance” of our faith has been the promise of an effective vaccine. We were told repeatedly by health policy experts and their talking heads in the media that an expectation of herd immunity, without the vaccine, was unrealistic and an irresponsible public policy which to promote. We were also told, unequivocally, in the absence of highly effective therapeutics to treat the virus, that a vaccine(s) was the only hope to defeat the virus and return to our previous lifestyles.
The “evidence” for the vaccine’s efficacy was shared with the world ahead of the rollout. And the evidence from the vaccine trials looked amazingly good, being around 95% effective at inducing an immune response. Even if real-world experience over time dilutes that number to 80%, that would still be very good compared to the efficacy of other vaccines in our arsenal against infectious diseases.
Most would agree, that’s pretty good “substance” on which to base our faith; but the reaction thus far from our leaders and experts seems baffling. Instead of being eager to validate the vaccine’s much anticipated protective immunity, their rhetoric and actions suggest nothing much has changed.
We have heard sparse talk about studies designed to validate immunity for those who have received the vaccine, but they still endorse it and promote its continued use. Other than that, it has been essentially the same pre-vaccine pandemic mantra: keep wearing masks, even in groups or families where everyone is immunized, and maintain a safe personal distance. There has been little conversation on whether the vaccine is even necessary (currently) in people who have had the natural disease; let alone about designing studies to answer that question.
Here is a vignette summarizing the state of the discourse as of February, 2021…
Co-Worker #1: “Have you received the COVID-19 vaccine yet?”.
Co-Worker #2: “No, I already had the virus in early December 2020 and recovered. I didn’t plan to get the vaccine, because I assume my immunity is pretty good right now, at least for a couple years, and that the vaccine probably won’t improve on that right now.”
Co-Worker #1: “But how do you know that?
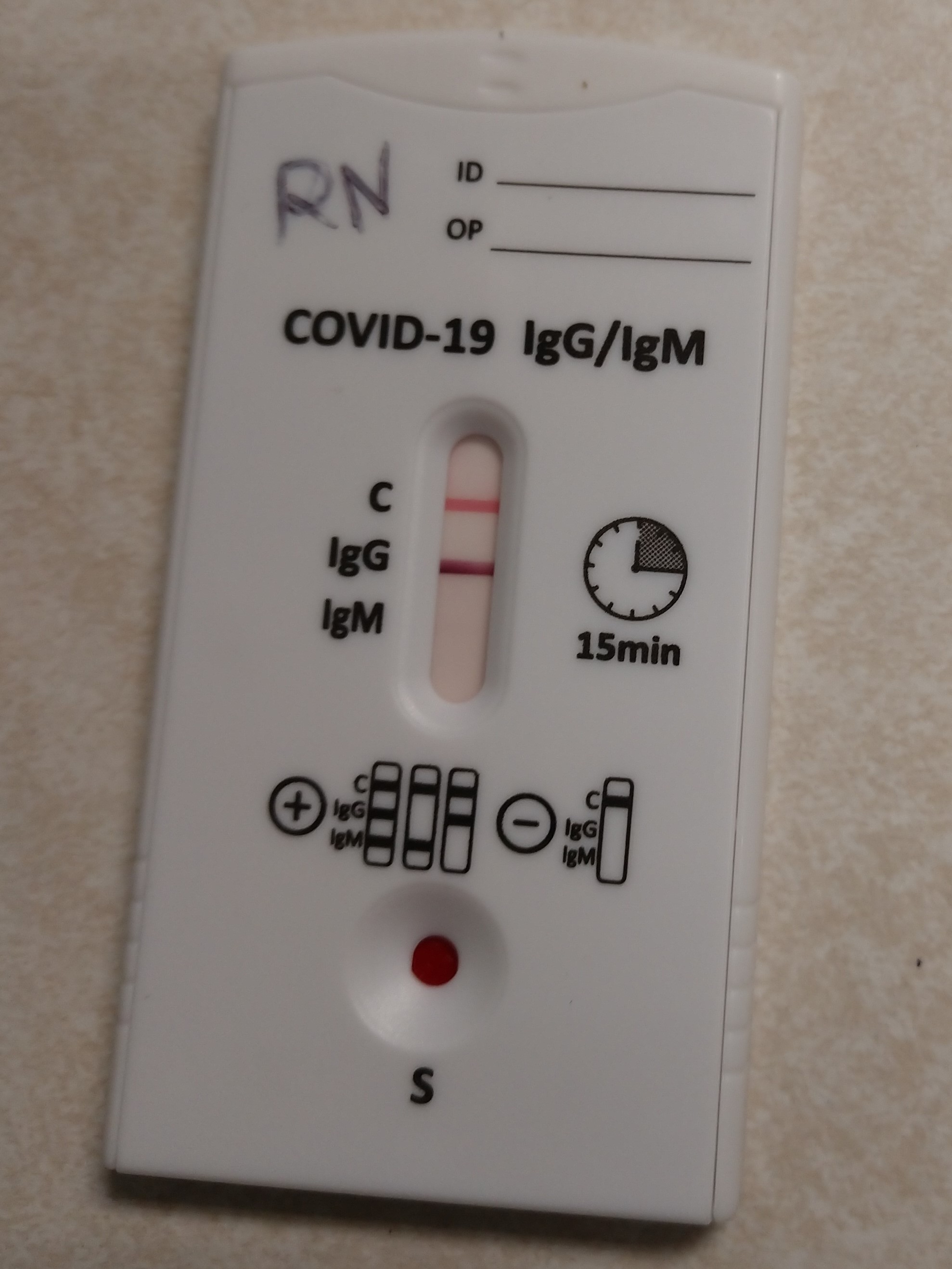
Co-Worker #2: “The question should be, why do we assume that a vaccine would be superior or add to my immunity? Several decades of viral illness research, immunity studies and vaccine studies indicate that recovering from a natural viral infection is typically the gold standard of immunity. And I have documented IgG antibody via a rapid test. My wife did not develop symptoms and tested negative for SARS-CoV-2 virus on two occasions shortly following my illness; and she tested negative for antibody.
We have a perfect opportunity to tease out the answers by compiling a rich set of data surrounding the issues debated by our two co-workers. We can answer these questions by making a few reasonable assumptions about viral illnesses and our immunity to them.
Assumption #1. For decades we have counseled patients that natural immunity (from having the disease) usually results in the best protection from repeat infection. Vaccines received within a few weeks or months following a natural infection are not thought to add significant advantages. There are some infectious diseases where vaccines appear to be superior to natural infection at triggering neutralizing antibody. However, neutralizing antibody is only one part of a comprehensive immune response; and the complexities of our body’s immune response to actual infection cannot be minimized. With few exceptions, after a given viral infection afflicts someone the first time, they develop protective immunity to it and rarely succumb to fully symptomatic infection a second time. Observation of this phenomenon, combined with serologic evidence, has made this a near cardinal doctrine in the practice of medicine.
Assumption #2. Viruses, unlike bacteria, are not thought to exist in a perpetual or prolonged state of carriage in asymptomatic persons. Most asymptomatic spread of COVID-19 is believed to take place in the those who are actually pre-symptomatic and where the virus is propagating and becoming infectious. While some patients remain truly asymptomatic (maybe 20% of infections) through the entire infection, the period of spreading infectious virus is NOT any longer, and possibly shorter, than compared to those who are in the pre-symptomatic/early symptomatic period. Unlike “Typhoid Mary”, who spread Salmonella Typhi bacteria to restaurant patrons, a person demonstrating immunity to COVID-19 virus would not be expected to harbor it in a contagious form indefinitely in their respiratory tract. Viruses, unlike bacteria, must over-take multiple host cells and then make copies of itself to propagate. Other than Herpes Simplex, Herpes Zoster, HIV and a couple other notable exceptions, viruses do not just hang out (contagious) in your body in dormant fashion.
“The relations between viral load, viral shedding, infection, infectiousness, and duration of infectiousness are not well understood. In a recent systematic review, no study was able to culture live virus from symptomatic participants after the ninth day of illness, despite persistently high viral loads in quantitative PCR diagnostic tests.” https://www.bmj.com/content/371/bmj.m4851
Assumption #3. Measurement of antibodies in the blood has long been accepted a reliable indicator of recovery from previous infection. Antibodies can be measured in qualitative assays (positive or negative) or in quantitative assays referred to as titers which provide a relative indicator of the level of antibody compared to background levels. Antibody titers are often used to gauge immune response to infection or the elapsed time since infection. Detectable serum IgM and/or IgG antibody has always been thought of as a surrogate marker of an adequate immune response – whether the result of a vaccine or natural disease; without the need to test all facets of the cellular immune response, which is tedious and expensive. Again, that does not mean that the antibody alone is adequate to neutralize the pathogen; but that the antibody is a marker that a person has recovered (usually) and that repeated infection would cause the immune system to act much quicker and effectively.
“Very few cases of reinfection with SARS-CoV-2 have been documented worldwide. Because the virus is so widespread, if getting infected didn’t give at least some protection, you’d expect many more people to have gotten the virus twice.8Also, studies have indicated that people with symptoms of COVID-19 seem to produce antibodies—effective, “neutralizing” antibodies (as assessed in a lab). From our experience with other viruses, we think that that means that getting infected with COVID-19 probably leads to at least some level of protection against future infection.8 “ https://www.verywellhealth.com/antibodies-from-vaccines-and-from-natural-infection-5092564
The nexus of those recently infected with the those who are newly immunized has created a brief window of time in which to examine precious data that will never exist again in its current form. What percentage of vaccine recipients get antibody? What percentage of those with natural disease get antibody? How long does it persist? Is the antibody protective and for how long? How does the immune response compare between the vaccine and those who contract the infection?
Designing these studies is not complicated. Our larger health systems around the country, the same ones charged with distributing the vaccine, are in a perfect position to lead these investigations. They have a relatively large percentage of employees who contracted the virus and a large percentage of employees who have received the vaccine; and some who had the disease AND receive the vaccine. They have the personnel, supplies and resources to carry out the studies.
What do we want our post-pandemic/post-vaccine world to look like? For me, I prefer to see entire faces; I miss smiles. I see people in the hallway on a regular basis and I have never seen their face uncovered! I want to experience handshakes and hugs, sooner rather than later!